
Unique Access provides access to an extensive treatment protocol for Brain Injuries by using higher quantities of stem cells, extensive rehabilitation, and many supportive therapies. This effective combination of the most advanced medical technologies, with systematic physical and occupational therapies, has helped previously treated patients achieve approved motor skills and other important gains.
Why Stem Cells Work for Traumatic Brain Injury (TBI)
The most prevalent and debilitating features in survivors of brain trauma are cognitive deficits and motor dysfunctions. To date, there is no effective treatment that promotes functional recovery except for routine medical intervention and care.
Fortunately, there are many emerging and promising drug- or cell-based therapeutic approaches. They include erythropoietin and its carbamylated form, statins, and stem cells treatment.
Novel treatment methods help to reduce brain injury via neuroprotection and promote brain remodeling via angiogenesis, neurogenesis, and synaptogenesis with a final goal of improving the functional outcome of Traumatic Brain Injury patients.
Possible Improvements
Patients that presented with Traumatic Brain Injury (TBI) had cases that ranged from mild to severe. Unique Access provides access to an extensive treatment protocol which uses a combination of Mesenchymal Stem Cells (MSCs), extensive rehab, and supportive therapies. Many of these patients have seen great treatment outcomes.
TBI patients treated with stem cells usually observe improvements in the following areas:
- Motor function
- Muscle tone and strength
- Cognition and memory
- Speech and swallowing
- Balance and coordination
- Fine motor skills
- Gross motor skills and more
Mechanisms
Stem cell treatment for Traumatic Brain Injury (TBI) will focus on the secondary brain injury, which is the result of biochemical and physiological events, ultimately leading to neuronal cell death.
Recent research has indicated that the potential therapeutic benefit of stem cell therapy could be the result of the following mechanisms:
1. Secrete growth factors to promote functional outcome after brain injury via neurogenesis and
synaptogenesis;
2. Produce and induce many cytokines and trophic factors to enhance angiogenesis and vascular stabilisation in the lesion boundary zone;
3. Decrease glial scar formation and promote glial-axonal remodeling;
4. Differentiate into cells of neural origin including neurons, astrocytes, and glial cells.
Stem cells therefore act in a pleiotropic way to stimulate brain remodeling after brain injury by influencing several neural restorative functions such as synaptogenesis, angiogenesis, and neurogenesis.
Our Promise
We believe that there is always hope and that patients deserve access to effective and safe treatments.
We are independent with an in-house medical department.
We combine internationally accredited hospitals, next generation treatments, unique products and services that are integrative and effective to ensure best possible treatment results.
Stem Cells
In terms of stem cells we will make sure that the patient will receive the correct and necessary stem cell type, quality, quantity and viability.
Our exclusive research partner guarantee a stem cell viability of 95%, many injections have a staggering viability of 98-99%.
Supportive Therapies & Remedies
- Hyperbaric Oxygen Chamber (HBOT)
- Hemo Oxygen Therapy (HOT)
- IV Vitamin Drips
- Immune-Boosting Supplements (e.g. GcMAF)
Partner Hospital
The treatment will take place in an internationally accredited tertiary care hospital and not in a hotel or clinic. This is important for the patient’s safety and care as the patient will have access to all specialized departments & specialist doctors which will further increase the treatments efficiency.
What is Traumatic Brain Injury?
Traumatic Brain Injury (TBI) is a general term referring to many different types of injuries which include, but are not limited to: cranial trauma, brain infections, and hypoxic-ischemic brain injuries.
Traumatic Brain Injury (TBI) is brain damage that results in the disruption or loss of some of its functions. In the US alone, approximately 2 million cases of mild-to-moderate Traumatic Brain Injury go unreported yearly, with 1.7 million people being admitted into hospitals and resulting in annual deaths of 50,000 per year. Usually, automobile accidents, falls, assaults/blows, sports-related injuries, and explosive blasts are common causes of TBI. Clinically, TBI concludes the primary brain injury and the secondary brain injury. Primary damage results from mechanical forces applied to the skull and brain at the time of impact, leading to focal or diffuse brain injury patterns.
In contrast to the primary injuries, secondary brain injuries evolve over time. These are characterised by a complex cascade of molecular and biochemical events that lead to neuroinflammation, brain edema, and delayed euronal death.

Common symptoms of Traumatic Brain Injury (TBI)
After Traumatic Brain Injury (TBI), persons often report symptoms in the days, weeks, and perhaps months following injury, but do improve over time. The most common symptoms after brain injury are known as Post-concussion Syndrome (PCS).
- Physical complaints
- Dizziness
- Fatigue
- Headaches
- Visual disturbances
- Trouble sleeping
- Sensitivity to light and sound
- Poor balance
- Cognitive changes
- Poor concentration
- Memory problems
- Poor judgment and impulsivity
- Slowed performance
- Difficulty putting thoughts into words
- Psychosocial concerns
- Depression
- Anger outbursts
- Irritability
- Personality changes
- Anxiety
More severe Traumatic Brain Injuries (TBIs) result in significant cognitive impairment, loss of motor function, impaired sensation, increased or decreased muscle tone, and may involve severe vision loss.
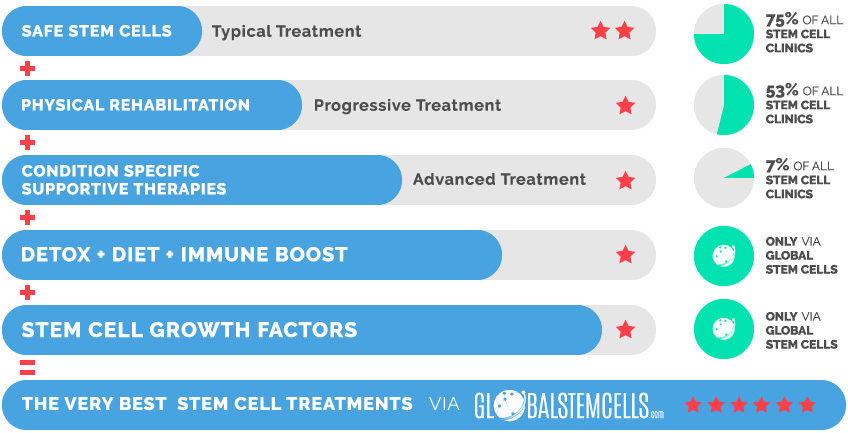
The Very Best Stem Cell Treatments via globalstemcells.com
- Rehman T, Ali R, Tawil I, Yonas H (2008).
“Rapid progression of traumatic bifrontal contusions to transtentorial herniation: A case report”. Cases journal. 1 (1): 203. doi: 10.1186/1757-1626-1-203. PMC 2566562. PMID 18831756.
- Maas AI, Stocchetti N, Bullock R (August 2008).
“Moderate and severe traumatic brain injury in adults”. Lancet Neurology. 7 (8): 728–41. doi: 10.1016/S1474-4422(08)70164-9. PMID 18635021.
- Parikh S, Koch M, Narayan RK (2007).
“Traumatic brain injury”. International Anesthesiology Clinics. 45 (3): 119–35. doi: 10.1097/AIA.0b013e318078cfe7. PMID 17622833.
- Collins C, Dean J (2002).
“Acquired brain injury”. In Turner A, Foster M, Johnson SE. Occupational Therapy and Physical Dysfunction: Principles, Skills and Practice. Edinburgh: Churchill Livingstone. pp. 395–96. ISBN 0-443-06224-2. Retrieved 2008-11-13.
- Ghajar J (September 2000).
“Traumatic brain injury”. Lancet. 356 (9233): 923–29. doi: 10.1016/S0140-6736(00)02689-1. PMID 11036909.
- Williams C, Wood RL (March 2010).
“Alexithymia and emotional empathy following traumatic brain injury”. J Clin Exp Neuropsychol. 32 (3): 259–67. doi: 10.1080/13803390902976940. PMID 19548166.
- Milders, M.; Fuchs, S.; Crawford, J. R. (2003).
“Neuropsychological impairments and changes in emotional and social behaviour following severe traumatic brain injury”. Journal of Clinical & Experimental Neuropsychology. 25(2): 157–172. doi: 10.1076/jcen.25.2.157.13642.
- Bay E, McLean SA (February 2007).
“Mild traumatic brain injury: An update for advanced practice nurses”. Journal of Neuroscience Nursing. 39 (1): 43–51. doi: 10.1097/01376517-200702000-00009. PMID 17396538.
- Narayan RK, Michel ME, Ansell B, et al. (May 2002).
“Clinical trials in head injury”. Journal of Neurotrauma. 19 (5): 503–57. doi: 10.1089/089771502753754037. PMC 1462953. PMID 12042091.
- Jones E, Fear NT, Wessely S (November 2007).
“Shell shock and mild traumatic brain injury: A historical review”. The American Journal of Psychiatry. 164 (11): 1641–5. doi: 10.1176/appi.ajp.2007.07071180. PMID 17974926.
External Links
- Brain Injury The official research journal of the International Brain Injury Association (IBIA)
- Cochrane Injuries Group: systematic reviews on the prevention, treatment and rehabilitation of traumatic injury
- First aid advice for head injuries from the British Red Cross
- Minor head injury and concussion information from Headway – the brain injury association
- The Brain Injury Hub – information and practical advice to parents and family members of children with acquired brain injury


 English
English